A study published on March 18 2025 in Pulmonary Therapy provides a comprehensive view of pulmonary hypertension in Japan through a nationwide survey of 160 patients (119 with pulmonary arterial hypertension (PAH) and 41 with chronic thromboembolic pulmonary hypertension (CTEPH) and 211 physicians.
We are particularly pleased to publish this article as one of the authors is Ms Noriko Murakami, Chairperson of PHA Japan, and mother of a patient.
In the pulmonary arterial hypertension group, the majority of patients (63 patients, 52.9%) were aged 41–60 years, and in the chronic thromboembolic pulmonary hypertension group most patients (20 patients, 48.8%) were aged 61–80 years. Idiopathic or heritable pulmonary arterial hypertension was the most common subtype in the pulmonary arterial hypertension group (67 patients, 56.3%). Stratification by WHO-FC among all patients with pulmonary arterial hypertension and chronic thromboembolic pulmonary hypertension showed that functional class (FC) II was most common type (80 patients, 50.0%), followed by FC I (37 patients, 23.1%), FC III (24 patients, 15.0%), and FC IV (3 patients, 1.9%). Patients were from various regions in Japan, with approximately 90% receiving care at pulmonary hypertension centers.
Among the physicians participating in the survey, most specialized in cardiology (34.6%), followed by respiratory medicine (25.1%) and rheumatology (14.2%). Over one half of participating physicians had > 5 years of experience treating pulmonary hypertension, and approximately 30% of pulmonary arterial hypertension physicians and 10% of chronic thromboembolic pulmonary hypertension physicians had treated ≥ 6 patients in the previous year. About 50% of physicians were affiliated with pulmonary hypertension centers.
Findings reveal diagnostic delays averaging 18 months from symptom onset, with patients visiting approximately 2.3 medical facilities before diagnosis. One of the aspects that emerged from the survey is the employment rates dropped significantly, from 68.8% pre-diagnosis to 36.9% at the time of survey, highlighting pulmonary hypertension’s substantial impact on patients’ livelihoods. Additionally, concerning communication gaps between patients and physicians were identified, particularly regarding treatment goals for chronic thromboembolic pulmonary hypertension patients.
The study demonstrates that Japanese patients face multiple challenges, including delayed diagnosis, employment difficulties, and communication barriers with healthcare providers. Health-related quality of life scores showed significant impairment that worsened with disease progression. The authors conclude that there is an urgent need for earlier diagnosis, better support systems for education and employment, and improved patient-physician communication to reduce disease burden and enhance outcomes for those living with this rare but severe condition.
Read more at this link on Pulmonary Therapy
Citation
Murakami, N., Asano, D., Tokushige, N. et al. Diagnostic Delays and Quality of Life in Japanese Patients with Pulmonary Hypertension: A Nationwide Survey. Pulm Ther (2025). https://doi.org/10.1007/s41030-025-00290-6
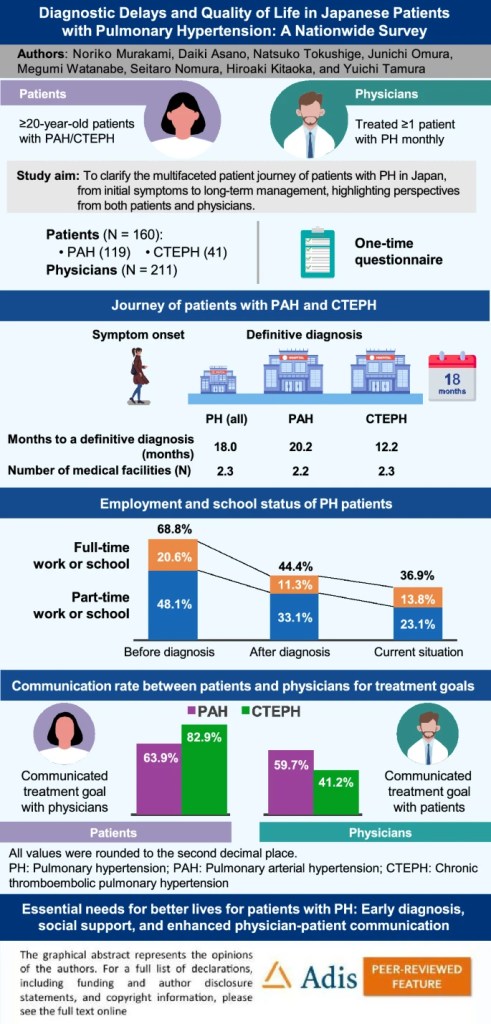
Photo credit: Article on Pulmonary Therapy

